Abstract
Cancer cells need extensive energy supply for their uncontrolled cell division and metastasis which is exclusively dependent on neighboring cells, especially adipocytes. Herein, we have introduced a novel herbometallic nano-drug, Heerak Bhasma nanoparticle (HBNP) from natural resources showing high potential in the reduction of energy supply thereby promoting cell death in breast cancer cells. Inductively coupled plasma optical emission spectra (ICP-OES), atomic absorption spectra (AAS), Raman spectra, X-ray diffraction analyses confirmed the physicochemical properties of HBNP. The differential light scattering (DLS) and field emission scanning electron microscope (FESEM) analyzed the cell-permeable size of HBNP, whereas, cell viability assay confirmed the non-toxic effect. Seahorse energy efflux assay, apoptotic cell quantification, ROS, mitochondrial membrane potential, in vivo oxidative stress etc. were measured using standard protocol. The notable changes in cancer energy metabolism investigated by cellular Mito and Glyco-stress analyses confirmed the HBNP induced intracellular energy depletion. Also, a significant reduction in mitochondrial membrane potential and subsequently, extensive reactive oxygen species (ROS) generations were observed in presence of HBNP followed by the induction of cell apoptosis. The cell invasion and wound healing assay followed by reduced expression both protein (MMP 2, MMP 9) and cytokine (IL6, IL10) had signified the effectiveness of HBNP against cancer metastasis. In addition, HBNP also showed an excellent antitumor activity in vivo followed by developing healing characteristics due to oxidative stress. All these findings strongly suggest that HBNP has the potential to be the new cancer therapeutic.
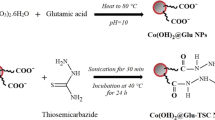
Graphic abstract
A schematic phenomenon represents the overall HBNP mediated anticancer activity via limitation of both fatty acid uptake and energy metabolism.










Similar content being viewed by others
References
Alderden RA, Hall MD, Hambley TW (2006) The discovery and development of cisplatin. J Chem Educ 83:728. https://doi.org/10.1021/ed083p728
Alessio E, Guo Z (2017) Metal anticancer complexes—activity, mechanism of action, future perspectives. Eur J Inorg Chem 2017:1539–1540. https://doi.org/10.1002/ejic.201700196
Aung TN, Qu Z, Kortschak RD, Adelson DL (2017) Understanding the effectiveness of natural compound mixtures in cancer through their molecular mode of action. Int J Mol Sci 18:656. https://doi.org/10.3390/ijms18030656
Bhattacharya B (2011) Elucidating the nanomaterialistic basis for Ayurvedic Bhasmas using physicochemical experimentation. J Biomed Nanotechnol 7:66–67. https://doi.org/10.1166/jbn.2011.1204
Buege JA, Aust SD (1978) Microsomal lipid peroxidation. Methods Enzymol 52:302–310. https://doi.org/10.1016/S0076-6879(78)52032-6
Chaudhury SS, Sannigrahi A, Nandi M, Mishra VK, De P, Chattopadhyay K, Mishra S, Sil J, Das Mukhopadhyay C (2019) A novel PEGylated block copolymer in new age therapeutics for Alzheimer disease. Mol Neurobiol 56:6551–6565. https://doi.org/10.1007/s12035-019-1542-1
Das N, Mandala AR, Naaz S, Giri S, Jain M, Bandyopadhyay D, Reiter RJ, Roy SS (2017) Melatonin protects against lipid induced mitochondrial dysfunction in hepatocytes and inhibit stellate cell activation during hepatic fibrosis in mice. J Pineal Res 62:12404. https://doi.org/10.1111/jpi.12404
Datta S, Choudhury D, Das A, Mukherjee DD, Das N, Roy SS, Chakraborty G (2017) Paclitaxel resistance development is associated with biphasic changes in reactive oxygen species, mitochondrial membrane potential and autophagy with elevated energy production capacity in lung cancer cells: a chronological study. Tumor Biol 39:694314. https://doi.org/10.1177/1010428317694314
Desoize B (2004) Metals and metal compounds in cancer treatment. Anticancer Res 24:1529–1544
Efferth T, Kahl S, Paulus K, Adams M, Rauh R, Boechzelt H, Hao X, Kaina B, Bauer R (2008) Phytochemistry and pharmacogenomics of natural products derived from traditional Chinese medica with activity against tumor cells. Mol Cancer Ther 7:152–161. https://doi.org/10.1158/1535-7163.MCT-07-0073
Egorova KS, Ananikov VP (2017) Toxicity of metal compounds: knowledge and myths. Organometallics 36:4071–4090. https://doi.org/10.1021/acs.organomet.7b00605
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82:48670–48677. https://doi.org/10.1016/0003-9861(59)90090-6
Erez A, DeBerardinis RJ (2015) Metabolic dysregulation in monogenic disorders and cancer—finding method in madness. Nat Rev Cancer 15:440–448. https://doi.org/10.1038/nrc3949
Esteva PFJ, Hubbard-Lucey VM, Tang J, Pusztai L (2019) Immunotherapy and targeted therapy combinations in metastatic breast cancer. Lancet Oncol 20:175–186. https://doi.org/10.1016/S1470-2045(19)30026-9
Geran RI, Greenberg NH, Mcdonald MM, Schumacher AM, Abbott BJ (1972) Protocols for screening chemical agents and natural products against animal tumors and other biological systems. Cancer Chemother. Rep 13:1. http://pascal-francis.inist.fr/vibad/index.php?action=getRecordDetail&idt=PASCAL733308013
Gorrini C, Harris IS, Mak TW (2013) Modulation of oxidative stress as an anticancer strategy. Nat Rev Drug Discov 12:931–947. https://doi.org/10.1038/nrd4002
Hambley TW (2007) Chemistry. Metal-based therapeutics. Science 318:1392. https://doi.org/10.1126/science.1150504
Joshi VK, Joshi A, Dhiman KS (2017) The Ayurvedic Pharmacopoeia of India, development and perspectives. J Ethnopharmacol 197:32–38. https://doi.org/10.1016/j.jep.2016.07.030
Joyce JA, Pollard JW (2009) Micro-environmental regulation of metastasis. Nat Rev Cancer 9:239–252. https://doi.org/10.1038/nrc2618
Jungwrith U, Kowol RC, Keppler BK, Hartinger CG, Berger W, Heffeter P (2011) Anticancer activity of metal complexes: involvement of redox processes. Antioxid Redox Signal 15:1085–1127. https://doi.org/10.1089/ars.2010.3663
Kamath SU, Pemiah B, Sekar RK, Krishnaswami S, Sethuraman S, Krishnan UM (2012) Mercury-based traditional herbo-metallic preparations: a toxicological perspective. Arch Toxicol 86:831–838. https://doi.org/10.1007/s00204-012-0826-2
Kono Y (1978) Generation of superoxide radical during auto-oxidation of hydroxylamine and an assay for superoxide dismutase. Arch Biochem Biophys 186:189–195. https://doi.org/10.1016/0003-9861(78)90479-4
Kramer N, Walzl A, Unger C, Rosner M, Krupitza G, Hengstschlager M, Dolznig H (2013) In-vitro cell migration and invasion assays. Mutat Res 752:10–24. https://doi.org/10.1016/j.mrrev.2012.08.001
Lee HS, Ha AW, Kim WK (2012) Effect of resveratrol on the metastasis of 4T1 mouse breast cancer cells in vitro and in vivo. Nutr Res Pract 6:294–300. https://doi.org/10.4162/nrp.2012.6.4.294
Liu J, Zhang F, Ravikanth V, Olajide OA, Li C, Wei LX (2019) Chemical compositions of metals in Bhasmas and Tibetan Zuotai are a major determinant of their therapeutic effects and toxicity. Evid Based Complement Altern Med 2019:2019. https://doi.org/10.1155/2019/1697804
Liu Y, Zhang P, Li F, Jin X, Li J, Chen W, Li Q (2018) Metal-based nanoenhancers for future radiotherapy: radiosensitizing and synergistic effects on tumor cells. Theranostics 8:1824–1849. https://doi.org/10.7150/thno.22172
Lopez-Soto A, Gonzalez S, Smyth MJ, Galluzzi L (2017) Control of metastasis by NK cells. Cancer Cell 32:135–154. https://doi.org/10.1016/j.ccell.2017.06.009
Lowry OH, Rosenbrough NJ, Farr FA, Randall RJ (1951) Protein measurement with the Folin’s phenol reagent. J Biol Chem 193:265–275. http://www.jbc.org/content/193/1/265.citation
Lv H, Zhen C, Liu J, Yang P, Hu L, Sang P (2019) Unraveling the potential role of glutathione in multiple forms of cell death in cancer therapy. Oxid Med Cell Longev 2019:3150145. https://doi.org/10.1155/2019/3150145
Martin DS, Bertino JR, Koutcher JA (2000) ATP depletion + pyrimidine depletion can markedly enhance cancer therapy: fresh insight for a new approach. Cancer 60:6776–6783. https://cancerres.aacrjournals.org/content/60/24/6776
Martinez-Outschoorn UE, Sotgia F, Lisanti MP (2012) Power surge: supporting cells “fuel” cancer cell mitochondria. Cell Metab 15:4–5. https://doi.org/10.1016/j.cmet.2011.12.011
Miao L, St Clair DK (2009) Regulation of superoxide dismutase genes: implications in disease. Free Radic Biol Med 47:344–356. https://doi.org/10.1016/j.freeradbiomed.2009.05.018
Millimouno FM, Dong J, Yang L (2014) Targeting apoptosis pathways in cancer and perspectives with natural compounds from mother-nature. Cancer Prev Res 7:1081–1107. https://doi.org/10.1158/1940-6207.CAPR-14-0136
Mjos KD, Orvig C (2014) Metallodrugs in medicinal inorganic chemistry. Chem Rev 114:4540–4563. https://doi.org/10.1021/cr400460s
Nafiujjaman M, Nurunnabi M, Saha SK, Jahan R, Lee YK, Rahmatullah M (2015) Anticancer activity of Arkeshwara Rasa—a herbometallic preparation. Ayu 36:346–350. https://doi.org/10.4103/0974-8520.182757
National Research Council (US) Committee for the Update of the Guide for the Care and Use of Laboratory Animals (2011), 8th edn. The National Academies Press, Washington, DC. ISBN-10: 0-309-15400-6
Nieboer E, Richardson DHS (1980) The replacement of the nondescript term ‘Heavy Metals’ by a biologically and chemically significant classification of metal ions. Environ Pollut B 1:3–26. https://doi.org/10.1016/0143-148X(80)90017-8
Nurgali K, Jogoe RT, Abalo R (2018) Editorial: adverse effects of cancer chemotherapy: anything new to improve tolerance and reduce sequelae? Front Pharmacol 9:245. https://doi.org/10.3389/fphar.2018.00245
Navya PN, Kaphle A, Srinivas SP, Bhargava SK, Rotello VM, Daima HK (2019) Current trends and challenges in cancer management and therapy using designer nanomaterials. Nano Converg 6:23. https://doi.org/10.1186/s40580-019-0193-2
Pal DK, Sahu CK, Haldar A (2014) Bhasma: the ancient Indian nanomedicine. J Adv Pharm Technol Res 5:4–12. https://doi.org/10.4103/2231-4040.126980
Palermo G, Magistrato A, Riedel T, von Erlach T, Davey CA, Dyson PJ, Rothlisberger U (2016) Fighting cancer with transition metal complexes: from naked DNA to protein and chromatin targeting strategies. ChemMedChem 11:1199–1210. https://doi.org/10.1002/cmdc.201500478
Parashar D, Geethadevi A, Aure MR, Mishra J, George J, Chen C, Mishra MK, Tahiri A, Zhao W, Nair B, Lu Y, Mangala LS, Rodriguez-Aguayo C et al (2019) miRNA551b-3p activates an oncostatin signaling module for the progression of triple-negative breast cancer. Cell Rep 29:4389–4406. https://doi.org/10.1016/j.celrep.2019.11.085
Parasuraman S, Thing GS, Dhanaraj SA (2014) Polyherbal formulation: concept of Ayurveda. Pharmacogn Rev 8:73–80. https://doi.org/10.4103/0973-7847.134229
Parida PK, Mahata B, Santra A, Chakraborty S, Ghosh Z, Raha S, Misra AK, Biswas K, Jana K (2018) Inhibition of cancer progression by a novel trans-stilbene derivative through disruption of microtubule dynamics, driving G2/M arrest, and p53-dependent apoptosis. Cell Death Dis 9:448. https://doi.org/10.1038/s41419-018-0476-2
Porporato PE, Filigheddu N, Pedro JNVS, Kroemer G, Galluzzi L (2018) Mitochondrial metabolism and cancer. Cell Res 28:265–280. https://doi.org/10.1038/cr.2017.155
Riccardi L, Genna V, De Vivo M (2018) Metal–ligand interactions in drug design. Nat Rev Chem 2:100–112. https://doi.org/10.1038/s41570-018-0018-6
Ruidas B, Chaudhary SS, Pal K, Sarkar PK, Das Mukhopadhyay C (2019) A novel herbometallic nanodrug has the potential for antibacterial and anticancer activity through oxidative damage. Nanomedicine 14:1173–1189. https://doi.org/10.2217/nnm-2018-0187
Sethi N, Kang Y (2011) Unravelling the complexity of metastasis—molecular understanding and targeted therapies. Nat Rev Cancer 11:735–748. https://doi.org/10.1038/nrc3125
Singh M, McGinley JN, Thompson HJ (2000) A comparison of the histopathology of premalignant and malignant mammary gland lesions induced in sexually immature rats with those occurring in the human. Lab Investig 80:221–231. https://doi.org/10.1038/labinvest.3780025
Sotgia F, Whitaker-Meneges D, Martinez-Outschoorn UE, Flomenberg N, Birbe R, Witkiewicz AK, Howell A, Philp NJ, Pestell RG, Lisanti MP (2012) Mitochondrial metabolism in cancer metastasis. Cell Cycle 11:1445–1454. https://doi.org/10.4161/cc.19841
Steeg PS (2016) Targeting metastasis. Nat Rev Cancer 16:201–218. https://doi.org/10.1038/nrc.2016.25
Swamy GYSK, Ravikumar K (2010) Characterization of Indian Ayurvedic herbal medicines for their metal concentrations using WD-XRF spectrometry. X-Ray Spectrom 39:216–220. https://doi.org/10.1002/xrs.1255
Trachootham D, Alexandre J, Huang P (2009) Targeting cancer cells by ROS mediated mechanism: a radical therapeutic approach? Nat Rev Drug Discov 8:579–591. https://doi.org/10.1038/nrd2803
Traverso N, Ricciarelli R, Nitti M, Marengo B, Furfaro AL, Pronzato ML, Marinari UM, Domenicotti C (2013) Role of glutathione in cancer progression and chemoresistance. Oxid Med Cell Longev 2013:972913. https://doi.org/10.1155/2013/972913
Uddin AH, Khalid RS, Alaama M, Abdualkader AM, Kasmuri A, Abbas SA (2016) Comparative study of three digestion methods for elemental analysis in traditional medicine products using atomic absorption spectrometry. J Anal Sci Technol 7:6. https://doi.org/10.1186/s40543-016-0085-6
Vera-Ramirez L, Sanchez-Rovira P, Ramirez-Tortosa MC, Ramirez-Tortosa CL, Granados-Principal S, Lorente JA, Quiles JL (2011) Free radicals in breast carcinogenesis, breast cancer progression and cancer stem cells; biological bases to develop oxidative-based therapies. Crit Rev Oncol Hematol 80:347–368. https://doi.org/10.1016/j.critrevonc.2011.01.004
Verrax J, Dejeans N, Sid B, Glorieux C, Calderon PB (2011) Intracellular ATP levels determine cell death fate of cancer cells exposed to both standard and redox chemotherapeutic agents. Biochem Pharmacol 82:1540–1548. https://doi.org/10.1016/j.bcp.2011.07.102
Vinay DS, Ryan EP, Pawelec G, Talib WH, Stagg J, Elcord T, Lichtor T, Decker WK, Whelan RL, Kumara HMCS et al (2015) Immune evasion in cancer: mechanistic basis and therapeutics strategies. Semin Cancer Biol 35:S185–S198. https://doi.org/10.1016/j.semcancer.2015.03.004
Vyas S, Zaganjor E, Haigis MC (2016) Mitochondria and cancer. Cell 166:555–566. https://doi.org/10.1016/j.cell.2016.07.002
Wang Y, Xia Y, Lu Z (2018) Metabolic features of cancer cells. Cancer Commun 38:65. https://doi.org/10.1186/s40880-018-0335-7
Warburg O, Wind F, Negelein E (1927) The metabolism of tumors in the body. J Gen Physiol 8:519–530. https://doi.org/10.1085/jgp.8.6.519
Weinhouse S (1956) On respiratory impairment in cancer cells. Science 124:267–269. https://doi.org/10.1126/science.124.3215.267
Webb AH, Gao BT, Goldsmith ZK, Irvine AS, Saleh N, Lee RP, Lendermon JB, Bheemreddy R, Zhang Q, Brennan RC, Johnson D, Steinle JJ, Wilson MW, Morales-Tirado VM (2017) Inhibition of MMP-2 and MMP-9 decreases cellular migration, and angiogenesis in in-vitro models of retinoblastoma. BMC Cancer 17:434. https://doi.org/10.1186/s12885-017-3418-y
Xiang Y, Guo Z, Zhu P, Chen J, Huang Y (2019) Traditional Chinese medicine as a cancer treatment: modern perspectives of ancient but advanced science. Cancer Med 8:1958–1975. https://doi.org/10.1002/cam4.2108
Acknowledgements
We acknowledge Dr. Punarbasu Chaudhury of the University of Calcutta (CU, India) for ICP-OES analysis and Dr. Sib Sankar Roy of Indian Institute of Chemical Biology (CSIR-IICB, India) for Seahorse Mito and Glyco-stress analysis. We thank Professor Parimal Karmakar of Jadavpur University (JU, India) for mitochondrial membrane potential investigation and Dr. Anjan Adhikari of R. G. Kar Medical College and Hospital, Kolkata, India for animal experiment facilities.
Funding
None to mention.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ruidas, B., Sur, T.K., Pal, K. et al. Herbometallic nano-drug inducing metastatic growth inhibition in breast cancer through intracellular energy depletion. Mol Biol Rep 47, 3745–3763 (2020). https://doi.org/10.1007/s11033-020-05467-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-020-05467-7