Abstract
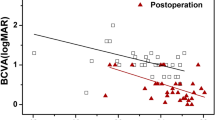
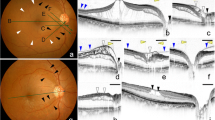
• Background: Vitreous surgery for idiopathic macular holes can result in both anatomic closure of the hole and visual improvement. In some patients even normal visual acuity is achieved. Postoperative visual field loss is a newly recognized complication. This prospective study evaluates the frequency and significance of scotomas after vitrectomy with gas tamponade for stage I–IV macular holes. • Methods: Over a period of 10 months, a consecutive series of 30 patients and 31 eyes with macular holes underwent pre- and postoperative automatic perimetry (Octopus 07, 70°) and macular perimetry (Octopus Ml, 24°) to characterize the pattern of visual field defects after vitrectomy with gas tamponade. Success rates were evaluated and complications were analyzed. • Results: Anatomic success after one surgical procedure was achieved in 85% of cases, visual improvement in 58%. Some 70.1% of patients had peripheral scotomas postoperatively; some of these were highly symptomatic and others were detected by visual field testing only. The most consistently affected areas were the temporal and lower periphery of the visual field. The central visual field, however, was not disturbed. • Conclusion: Visual field loss after otherwise successful surgery for macular holes is an unexpectedly frequent and serious complication. The authors discuss various factors that may contribute to the postoperative scotomas. From the localization of the scotomas it seems most likely that they are caused by the persistent pressure of the gas bubble on the peripheral retina. Further investigations are necessary to confirm this hypothesis, and ways must be found to avoid this complication in order to be able to proceed with this otherwise promising new indication group for vitreous surgery.
Similar content being viewed by others
References
Chang S, Sparrow JR, Iwamoto T, Gershbein A, Ross R, Ortiz R (1991) Experimental studies of tolerance to intravitreal perfluoro-N-octane liquid. Retina 11:367–374
Charles S (1993) Retinal pigment epithelial abnormalities after macular hole surgery. Retina 13: 176
Duker IS (1993) Retinal pigment epitheliopathy after macular hole surgery. Ophthalmology 100: 1604–1605
Duker JS (1994) Late re-opening of macular holes after initially successful treatment with vitreous surgery. Ophthalmology 101: 1373–1378
Eckhardt U, Eckardt C (1995) Binokularsehen bei idiopathischen Makulaforamen. Ophthalmologe 92:626–630
Eckhardt C, Nikolai U, Winter M, Knop E (1991) Experimental intraocular tolerance to liquid perfluorooctane and poly fluoropolyether. Retina 11:375–384
Eisner G (1985) Clinical anatomy of the vitrous. In: Duane TD, Jaeger EA (eds) Biomedical foundations of ophthalmology, vol 1, chap 16. Harper & Row, Philadelphia, pp 23–29
Fineberg E, Machemer R, Sullivan P, et al (1975) Sulfur hexafluoride in the owl monkey vitreous cavity. Am J Ophthalmol 79: 67–76
Foos RY, Roth AM (1973) Surface structure of the optic nerve head. 2. Vitreopapillary attachments and posterior vitreous detachment. Am J Ophthalmol 76: 662–671
Funata M, Wendel RT, de la Cruz Z, Green WR (1992) Clinicopathologic study of bilateral macular holes treated with pars plana vitrectomy and gas tamponade. Retina 12: 289–298
Gass JDM (1988) Idiopathic senile macular hole. Its early stages and pathogenesis. Arch Ophthalmol 106: 629–639
Gass JDM (1995) Reappraisal of biomicroscopic classification of stages of development of a macular hole. Am J Ophthalmol 119: 752–759
Gonvers M, Homung JP, de Courten C (1986) The effect of liquid silicone on the rabbit retina: histologic and ultrastructural study. Arch Ophthalmol 104: 1057–1062
Guyer DR, Green WR, de Bustros S, Fine SL (1989) Histopathologic features of idiopathic macular holes and cysts. Ophthalmology 97: 1045–1051
Hee MR, Puliafito CA, Wong C, Duker JS, Reichel E, Schuman JS, Swanson EA, Fujimoto JG (1995) Optical coherence tomography of macular holes. Ophthalmology 102: 748–756
Inderfurth J, Eckhardt C (1996) Neue Lagerung nach Netzhaut-Chirurgie mit Gas. Paper and abstract presented at 9th Annual Meeting of Retinologische Gesellschaft, Munich, 29 July
Kelly NE, Wendel RT (1991) Vitreous surgery for idiopathic macular holes: results of a pilot study. Arch Ophthalmol 109: 654–659
Kerrison JB, Haller JA, Elman M, Miller NR (1996) Visual field loss following vitreous surgery. Arch Ophthalmol 114: 564–569
Knorr HLJ, Seltsam A, Holbach L, Naumann GOH (1996) Intraokuläre Silikonöltamponade: eine klinischpathologische Studie an 36 enukleierten Augen. Ophthalmologe 93: 130–138
Lansing MB, Glaser BM, Liss H, Hanham A, Thompson JT, Sjaarda RN, Goron AJ (1993) The effect of pars plana vitrectomy and transforming growth factor-beta 2 without epiretinal membrane peeling on full-thickness macular holes. Ophthalmology 100: 868–872
Liggett PE, Skolik SA, Horio B, Saito Y, Alfaro V, Mieler W (1995) Human autologous serum for the treatment of full-thickness macular holes: a preliminary study. Ophthalmology 102: 1071–1076
Lincoff H, Kreissig I (1981) Intravitreal behaviour of perfluorocarbons. Dev Ophthalmol 2: 17–23
Lincoff H, Mardissian J, Lincoff A, et al (1980) Intravitreal longevity of three perfluorocarbon gases. Arch Ophthalmol 98: 1610–1611
Lincoff H, Coleman J, Kreissig I et al. (1983) The perfluorocarbon gases in the treatment of retinal detachment. Ophthalmology 90: 546–551
Lincoff H, Kreissig I, Jakobiec F, Vitolo J, Shapiro R (1986) Gas vitrectomy in a primate model. Graefe's Arch Clin Exp Ophthalmol 224: 215–217
Madreperla SA, Geiger GL, Funata M, et al. (1994) Clinicopathologic correlation of a macular hole treated by cortical vitreous peeling and gas tamponade. Ophthalmology 101:682–686
Mein CE, Flynn HW (1991) Recognition and removal of the posterior cortical vitreous during vitreoretinal surgery for impending macular hole. Am J Ophthalmol 111: 611–613
Melberg NS, Thomas MA (1995) Visual field loss after pars plana vitrectomy with air/fluid exchange. Am J Ophthalmol 120: 386–388
Orellana J, Liebermann RM (1993) Stage III macular hole surgery. Br J Ophthalmol 77: 555–558
Park SS, Marcus DM, Duker JS, Pesavento RD, Topping TM, Frederick AR, D'Amico DJ (1995) Posterior segment complications after vitrectomy for macular holes. Ophthalmology 102: 775–781
Pendergast SD, McCuen BW (1996) Visual field loss after macular hole surgery. Ophthalmology 103: 1069–1077
Poliner LS, Thomambe PE (1992) Retinal pigment epitheliopathy after macular hole surgery. Ophthalmology 99: 1671–1677
Polk TD, Smiddy WE, Flynn HW (1996) Bilateral visual function after macular hole surgery. Ophthalmology 103: 422–426
Puliafito CA, Hee MR, Lin CP, Reichel E, Schuman JS, Duker JS, Izatt JA, Swanson EA, Fujimoto JG (1995) Imaging of macular diseases with optical coherence tomography. Ophthalmology 102: 217–229
Ruby AJ, Williams DF, Grand MG, Thomas MA, Meredith TA, Boniuk I, Olk RJ (1994) Pars plana vitrectomy for treatment of stage 2 macular holes. Arch Ophthalmol 112: 359–364
Ryan EH, Gilbert HD (1994) Results of surgical treatment of recent-onset full-thickness idiopathic macular holes. Arch Ophthalmol 112: 1545–1553
Sjaarda RN, Glaser BM, Thompson JT, Murphy RP, Hanham A (1995) Distribution on iatrogenic retinal breaks in macular hole surgery. Ophthalmology 102: 1387–1392
Stolba U, Mudrich C, Krepler K, Velikay M, Binder S (1996) Der Effekt des spezifischen Gewichtes von Perfluorocarbonen auf die Netzhaut. Paper and abstract presented at 9th Annual Meeting of Retinologische Gesellschaft, Munich, 29 July
Thompson JT (1989) Kinetics of intraocular gases. Arch Ophthalmol 107: 687–691
Wendel RT, Patel AC, Kelly NE, Salzano TC, Wells JW, Novack GD (1993) Vitreous surgery for macular holes. Ophthalmology 100: 1671–1676
Wong RF, Thompson JT (1988) Prediction of the kinetics of disappearance of sulfur hexafluoride and perfluoropropane intraocular gas bubbles. Ophthalmology 95: 609–613
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bopp, S., Lucke, K. & Hille, U. Peripheral visual field loss after vitreous surgery for macular holes. Graefe's Arch Clin Exp Ophthalmol 235, 362–371 (1997). https://doi.org/10.1007/BF00937285
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00937285