Abstract
Purpose
To report the outcomes of implementing the ACOSOG Z0011 and AMAROS trials relevant to clinical practice, and to define target groups in whom to avoid or recommend axillary radiotherapy (ART). We also aimed to analyse the reduction in morbidity when axillary lymph node dissection (ALND) was omitted.
Methods
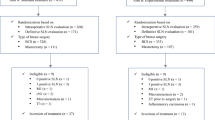
A retrospective cohort study of T1–T2 patients with macrometastases at sentinel lymph node (SLN) who were treated between 2011 and 2020. Breast surgery included either lumpectomy or mastectomy. Patients with ≤ 2 positive SLN were divided into two cohorts by whether they received ART or not. Survival outcomes and morbidity were analysed by Kaplan–Meyer curves and Cox-regression, respectively.
Results
260 pN1a patients were included and ALND was avoided in 167 (64.2%). According the Z0011 results, 72 (43.1%) received no further ART; and based on AMAROS criteria 95 (56.9%) received ART. Median follow-up was 54 months. The 5-year overall survival was 96.8% in the non-RT cohort and 93.4% in the RT cohort (p = 0.19), while the respective 5-year disease-free survivals were 100% and 92.3% (p = 1.06). Lymphedema developed in 3.6% of patients after SLNB versus 43% after ALND (OR 20.25; 95%CI 8.13–50.43). Decreased upper-extremity range of motion appeared in 8.4% of patients after SLNB versus 31.2% after ALND (OR 4.95; 95%CI 2.45–9.98%).
Conclusions
Our study confirms that omitting ALND is safe and has high survival rates in patients with T1–T2 tumours and ≤ 2 positive SLNs. Adding ART could be a treatment option for patients who present other risk factors. Avoiding ALND with or without ART was associated with significantly less arm morbidity.




Similar content being viewed by others
References
de Boniface J et al (2017) Survival and axillary recurrence following sentinel node-positive breast cancer without completion axillary lymph node dissection: The randomized controlled SENOMAC trial. BMC Cancer 17(1):1–7. https://doi.org/10.1186/s12885-017-3361-y
Giuliano AE et al (2017) Effect of axillary dissection vs no axillary dissection on 10-year overall survival among women with invasive breast cancer and sentinel node metastasis: the ACOSOG Z0011 (Alliance) randomized clinical trial. JAMA 318(10):918–926. https://doi.org/10.1001/jama.2017.11470
Donker M et al (2015) AMAROS trial. Lancet Oncol 15(12):1303–1310. https://doi.org/10.1016/S1470-2045(14)70460-7.Radiotherapy
Pilewskie M, Zabor EC, Mamtani A, Barrio AV, Stempel M, Morrow M (2017) The optimal treatment plan to avoid axillary lymph node dissection in early-stage breast cancer patients differs by surgical strategy and tumor subtype. Ann Surg Oncol 24(12):3527–3533. https://doi.org/10.1245/s10434-017-6016-y
Verheuvel NC, Voogd AC, Tjan-Heijnen VCG, Roumen RMH (2016) Potential impact of application of Z0011 derived criteria to omit axillary lymph node dissection in node positive breast cancer patients. Eur J Surg Oncol 42(8):1162–1168. https://doi.org/10.1016/j.ejso.2016.05.007
“The diagnosis and treatment of peripheral lymphedema: 2013 Consensus document of the international society of lymphology,” in Lymphology, March 2013, vol 46, no 1, p 1–11. [Online]. Available: https://pubmed.ncbi.nlm.nih.gov/23930436/. Accessed 21 Jan 2021
Giuliano AE et al (2011) Axillary dissection vs no axillary dissection in women with invasive breast cancer and sentinel node metastasis: a randomized clinical trial. JAMA 305(6):569–575. https://doi.org/10.1001/jama.2011.90
Giuliano AE et al (2010) Locoregional recurrence after sentinel lymph node dissection with or without axillary dissection in patients with sentinel lymph node metastases: the American college of surgeons oncology group z0011 randomized trial. Ann Surg 252(3):426–432. https://doi.org/10.1097/SLA.0b013e3181f08f32
Balic M, Thomssen C, Würstlein R, Gnant M, Harbeck N (2019) St. Gallen/Vienna 2019: a brief summary of the consensus discussion on the optimal primary breast cancer treatment. Breast Care. https://doi.org/10.1159/000499931
Mamtani A et al (2016) Age and receptor status do not indicate the need for axillary dissection in patients with sentinel lymph node metastases. Ann Surg Oncol 23(11):3481–3486. https://doi.org/10.1245/s10434-016-5259-3
Dengel LT et al (2014) Axillary dissection can be avoided in the majority of clinically node-negative patients undergoing breast-conserving therapy. Ann Surg Oncol 21(1):22–27. https://doi.org/10.1245/s10434-013-3200-6
Ong CT et al (2017) Patient Age and Tumor Subtype Predict the Extent of Axillary Surgery Among Breast Cancer Patients Eligible for the American College of Surgeons Oncology Group Trial Z0011. Ann Surg Oncol 24(12):3559–3566. https://doi.org/10.1245/s10434-017-6075-0
Whelan TJ et al (2015) Regional nodal irradiation in early-stage breast cancer. N Engl J Med 373(4):307–316. https://doi.org/10.1056/nejmoa1415340
Kataoka A et al (2016) Young adult breast cancer patients have a poor prognosis independent of prognostic clinicopathological factors: a study from the Japanese Breast Cancer Registry. Breast Cancer Res Treat 160(1):163–172. https://doi.org/10.1007/s10549-016-3984-8
Fisher B et al (2002) Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med 347(16):1233–1241. https://doi.org/10.1056/nejmoa022152
Sun YS et al (2017) Risk factors and preventions of breast cancer. Int J Biol Sci 13(11):1387–1397. https://doi.org/10.7150/ijbs.21635
Yang X, Ma XX, Yang W, Shui R (2020) Clinical significance of extranodal extension in sentinel lymph node positive breast cancer. Sci Rep. https://doi.org/10.1038/s41598-020-71594-7
Nottegar A et al (2016) Extra-nodal extension of sentinel lymph node metastasis is a marker of poor prognosis in breast cancer patients: a systematic review and an exploratory meta-analysis. Eur J Surg Oncol 42(7):919–925. https://doi.org/10.1016/j.ejso.2016.02.259
Van La Parra RFD, Peer PGM, Ernst MF, Bosscha K (2011) Meta-analysis of predictive factors for non-sentinel lymph node metastases in breast cancer patients with a positive SLN. Eur J Surg Oncol 37(4):290–299. https://doi.org/10.1016/j.ejso.2011.01.006
Salinas S (2019) Rehabilitación y cáncer de mama: factores de riesgo asociados a linfedema y limitación del hombro (Tesis doctoral). Programa Dr. en Med. i Recer. Translacional. Dep. Med. Univ. Barcelona
Wernicke AG et al (2013) Complication rates in patients with negative axillary nodes 10 years after local breast radiotherapy after either sentinel lymph node dissection or axillary clearance. Am J Clin Oncol Cancer Clin Trials 36(1):12–19. https://doi.org/10.1097/COC.0b013e3182354bda
Lee TS, Kilbreath SL, Refshauge KM, Herbert RD, Beith JM (2008) Prognosis of the upper limb following surgery and radiation for breast cancer. Breast Cancer Res Treat 110(1):19–37. https://doi.org/10.1007/s10549-007-9710-9
DiSipio T, Rye S, Newman B, Hayes S (2013) Incidence of unilateral arm lymphoedema after breast cancer: a systematic review and meta-analysis. Lancet Oncol 14(6):500–515. https://doi.org/10.1016/S1470-2045(13)70076-7
Hidding JT, Beurskens CHG, Van Der Wees PJ, Van Laarhoven HWM, Nijhuis-van Der Sanden MWG (2014) Treatment related impairments in arm and shoulder in patients with breast cancer: a systematic review. PLoS ONE. https://doi.org/10.1371/journal.pone.0096748
Monleon S, Murta-Nascimento C, Bascuas I, Macià F, Duarte E, Belmonte R (2015) Lymphedema predictor factors after breast cancer surgery: a survival analysis. Lymphat Res Biol 13(4):268–274. https://doi.org/10.1089/lrb.2013.0042
Acknowledgements
We thank Michael Maudsley, MSc, for language revision.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ortega Expósito, C., Falo, C., Pernas, S. et al. The effect of omitting axillary dissection and the impact of radiotherapy on patients with breast cancer sentinel node macrometastases: a cohort study following the ACOSOG Z0011 and AMAROS trials. Breast Cancer Res Treat 189, 111–120 (2021). https://doi.org/10.1007/s10549-021-06274-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-021-06274-9