Abstract
Study design
Prospective double-blind, randomized controlled trial.
Objectives
The objective of this study was to validate the efficacy of gabapentin as part of a multimodal pain regimen in a double-blind, randomized controlled trial for patients aged 10–19 years with idiopathic scoliosis undergoing posterior spinal fusion.
Summary of background data
Perioperative pain management represents a challenge for patients undergoing surgical correction of adolescent spinal deformity. Gabapentin has been shown to decrease postoperative pain and opioid use after spine surgery, but it has not yet been investigated as part of a multimodal pain regimen intended to decrease the perioperative use of opioids.
Methods
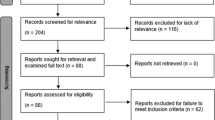
Fifty patients were randomized to receive gabapentin or placebo pre- and postoperatively in addition to a standardized medication regime including scheduled ketorolac and as-needed acetaminophen, hydromorphone, and oxycodone. Patients were monitored in the pre-, peri-, and postoperative periods for pain levels, medication dosing, side effects, adverse events, hospitalization length of stay, and parent satisfaction.
Results
There were statistically significant decreases in early postoperative pain scores and opioid use as well as total postoperative opioid use for the treatment group relative to controls. There were no statistically significant differences in adverse events, medication side effects, or hospitalization length. Parents of patients in both groups were very satisfied with the pain control provided to their children.
Conclusions
This randomized controlled trial demonstrates that pre- and postoperative administration of gabapentin as part of a multimodal pain management protocol significantly decreases both opioid use and visual analog pain scales in the first two postoperative days after posterior spinal fusion for adolescent idiopathic scoliosis. Gabapentin should be considered as a standard medication for perioperative pain control in this patient population.
Level of evidence
Level I.




Similar content being viewed by others
References
Inturrisi CE (2002) Clinical pharmacology of opioids for pain. Clin J Pain 18(4):S3–S13
McCabe SE, West BT, Boyd CJ (2013) Leftover prescription opioids and nonmedical use among high school seniors: a multi-cohort national study. J Adolesc Health 52:480–485
McCabe SE, West BT, Veliz P et al (2017) Trends in medical and nonmedical use of prescription opioids among US adolescents: 1976–2015. Pediatrics 139:e20162387–11
Kaye AD, Cornett EM, Helander E et al (2017) An update on nonopioids: intravenous or oral analgesics for perioperative pain management. Anesthesiol Clin 35:e55–e71
Rivkin A, Rivkin MA (2014) Perioperative nonopioid agents for pain control in spinal surgery. Am J Health Syst Pharm 71:1845–1857
Nowicki PD, Vanderhave KL, Gibbons K et al (2012) Perioperative pain control in pediatric patients undergoing orthopaedic surgery. J Am Acad Orthop Surg 20:755–765
Dunn LK, Durieux ME, Nemergut EC (2016) Non-opioid analgesics: novel approaches to perioperative analgesia for major spine surgery. Best Pract Res Clin Anaesthesiol 30:79–89
Milbrandt TA, Singhal M, Minter C et al (2009) A comparison of three methods of pain control for posterior spinal fusions in adolescent idiopathic scoliosis. Spine 34:1499–1503
Hiller A, Helenius I, Nurmi E et al (2012) Acetaminophen improves analgesia but does not reduce opioid requirement after major spine surgery in children and adolescents. Spine 37:E1225–E1231
Munro HM, Walton SR, Malviya S et al (2002) Low-dose ketorolac improves analgesia and reduces morphine requirements following posterior spinal fusion in adolescents. Can J Anesth 49:461–466
Sucato DJ, Lovejoy JF, Agrawal S et al (2008) Postoperative ketorolac does not predispose to pseudoarthrosis following posterior spinal fusion and instrumentation for adolescent idiopathic scoliosis. Spine 33:1119–1124
Hayes J, Pehora C, Bissonnette B (2009) The use of NSAIDs in pediatric scoliosis surgery—a survey of physicians’ prescribing practice. Paediatr Anaesth 19:756–763
Turan A, Karamanlioğlu B, Memiş D et al (2004) Analgesic effects of gabapentin after spinal surgery. Anesthesiology 100:935–938
Mayell A, Srinivasan I, Campbell F, Peliowski A (2014) Analgesic effects of gabapentin after scoliosis surgery in children: a randomized controlled trial. Paediatr Anaesth 24:1239–1244
Rusy LM, Hainsworth KR, Nelson TJ et al (2010) Gabapentin use in pediatric spinal fusion patients. Anesth Analg 110:1393–1398
Kong VKF, Irwin MG (2007) Gabapentin: a multimodal perioperative drug? Br J Anaesth 99:775–786
Gornitzky AL, Flynn JM, Muhly WT, Sankar WN (2016) A rapid recovery pathway for adolescent idiopathic scoliosis that improves pain control and reduces time to inpatient recovery after posterior spinal fusion. Spine Deform 4:288–295
Muhly WT, Sankar WN, Ryan K et al (2016) Rapid recovery pathway after spinal fusion for idiopathic scoliosis. Pediatrics 137:e20151568
Von Korff M, Korff MV, Saunders K et al (2008) De facto long-term opioid therapy for noncancer pain. Clin J Pain 24:521–527
Quinlan-Colwell A, Thear G, Miller-Baldwin E, Smith A (2017) Use of the Pasero Opioid-induced Sedation Scale (POSS) in pediatric patients. J Pediatr Nurs 33:83–87
Bailey B, Gravel J, Daoust R (2012) Reliability of the visual analog scale in children with acute pain in the emergency department. Pain 153:839–842
Farrar JT (2010) Advances in clinical research methodology for pain clinical trials. Nat Med 16:1284–1293
Acknowledgments
The authors thank Brandy Gonzalez and Jordan Cusick, research assistants with the OHSU Department of Pediatric Surgery, for their help in collecting and organizing clinical data. We also thank the perioperative and nursing staff at Doernbecher Children’s Hospital, who were diligent about incorporating the study protocol into their work. Finally, we thank the research pharmacy at OHSU, who randomized patients and formulated the study medication and placebo. No specific research funding was obtained for this project.
Funding
No specific funding was obtained for this investigation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
DEA (none), NTD (none), EBP (none), MFH (none).
Ethical standards
This study received institutional IRB approval (IRB no. 9681) and was registered with ClinicalTrials.org (NCT01977937) before patient enrollment.
IRB approval
This study received institutional IRB approval (IRB no. 9681) and was registered with ClinicalTrials.org (NCT01977937) before patient enrollment.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Anderson, D.E., Duletzke, N.T., Pedigo, E.B. et al. Multimodal pain control in adolescent posterior spinal fusion patients: a double-blind, randomized controlled trial to validate the effect of gabapentin on postoperative pain control, opioid use, and patient satisfaction. Spine Deform 8, 177–185 (2020). https://doi.org/10.1007/s43390-020-00038-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-020-00038-z