Abstract
Purpose
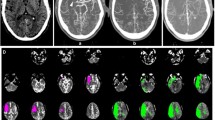
There is increasing use of automated computed tomography perfusion (CTP) to aid thrombectomy decision in emergent large vessel occlusion. It is important to understand the performance of these software packages in predicting ischemic core and tissue-at-risk in the real-world setting. The aim of this study was to evaluate whether ischemic core on non-contrast CT (NCCT) and automated CTP correspond and predict infarct extent after thrombectomy for ischemic stroke.
Methods
Consecutive patients with acute anterior circulation large vessel occlusion undergoing successful thrombectomy (TICI 2b/3) were studied. All patients had baseline CT, CTP with RAPID post-processing software (RAPID-CTP), and post-thrombectomy 24 h CT. Ischemic cores were assessed by two blinded raters independently using the Alberta Stroke Program Early Computed Tomography Score (ASPECTS) on each modality. The interrater agreement for ASPECTS, and correlation between baseline CT-ASPECTS, RAPID-CTP-ASPECTS, and 24h CT-ASPECTS were calculated.
Results
A total of 86 patients with a mean age of 70.3 years (SD 16.5) were studied. The median baseline CT-ASPECTS was 9.5 (interquartile range, IQR 8–10), median RAPID-CTP-ASPECTS was 9 (IQR 8–10), and mean RAPID-CTP-ischemic core volume was 14.4 ml (SD 27.9 ml). The mean mismatch volume (difference of Tmax > 6s and cerebral blood flow (CBF) < 30%) was 128.6 ml (SD 126.0 ml). There was substantial correlation between baseline and 24h CT-ASPECTS (rs: 0.62; p < 0.001), but poor correlation between RAPID-CTP-ASPECTS and RAPID-CTP ischemic core volume with 24h NCCT-ASPECTS (rs: 0.21; p = 0.06 and −0.16; p = 0.15 respectively). The positive predictive value of any established infarct for baseline CT-ASPECTS was 81%, while that of RAPID-CTP-ASPECTS was 64%.
Conclusion
In this series of successfully revascularized patients, ischemic core as estimated by RAPID-CTP-ASPECTS did not correlate with the baseline CT and tended to depict a larger infarct core than the infarct extent as assessed by 24h CT-ASPECTS.


Similar content being viewed by others
Abbreviations
- ASPECTS:
-
Alberta Stroke Program Early Computed Tomography Score
- ELVO:
-
Emergent large vessel occlusion
References
Albers GW, Lansberg MG, Kemp S, Tsai JP, Lavori P, Christensen S, Mlynash M, Kim S, Hamilton S, Yeatts SD, Palesch Y, Bammer R, Broderick J, Marks MP. A multicenter randomized controlled trial of endovascular therapy following imaging evaluation for ischemic stroke (DEFUSE 3). Int J Stroke. 2017;12:896–905.
Campbell BC, Mitchell PJ, Kleinig TJ, Dewey HM, Churilov L, Yassi N, Yan B, Dowling RJ, Parsons MW, Oxley TJ, Wu TY, Brooks M, Simpson MA, Miteff F, Levi CR, Krause M, Harrington TJ, Faulder KC, Steinfort BS, Priglinger M, Ang T, Scroop R, Barber PA, McGuinness B, Wijeratne T, Phan TG, Chong W, Chandra RV, Bladin CF, Badve M, Rice H, de Villiers L, Ma H, Desmond PM, Donnan GA, Davis SM; EXTEND-IA Investigators. Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med. 2015;372:1009–18.
Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, McTaggart RA, Torbey MT, Kim-Tenser M, Leslie-Mazwi T, Sarraj A, Kasner SE, Ansari SA, Yeatts SD, Hamilton S, Mlynash M, Heit JJ, Zaharchuk G, Kim S, Carrozzella J, Palesch YY, Demchuk AM, Bammer R, Lavori PW, Broderick JP, Lansberg MG; DEFUSE 3 Investigators. Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med. 2018;378:708-18.
Nogueira RG, Jadhav AP, Haussen DC, Bonafe A, Budzik RF, Bhuva P, Yavagal DR, Ribo M, Cognard C, Hanel RA, Sila CA, Hassan AE, Millan M, Levy EI, Mitchell P, Chen M, English JD, Shah QA, Silver FL, Pereira VM, Mehta BP, Baxter BW, Abraham MG, Cardona P, Veznedaroglu E, Hellinger FR, Feng L, Kirmani JF, Lopes DK, Jankowitz BT, Frankel MR, Costalat V, Vora NA, Yoo AJ, Malik AM, Furlan AJ, Rubiera M, Aghaebrahim A, Olivot JM, Tekle WG, Shields R, Graves T, Lewis RJ, Smith WS, Liebeskind DS, Saver JL, Jovin TG; DAWN Trial Investigators. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med. 2018;378:11–21.
Knoepfli AS, Sekoranja L, Bonvin C, Delavelle J, Kulcsar Z, Rüfenacht D, Yilmaz H, Sztajzel R, Altrichter S, Lövblad KO. Evaluation of perfusion CT and TIBI grade in acute stroke for predicting thrombolysis benefit and clinical outcome. J Neuroradiol. 2009;36:131–7.
Demeestere J, Garcia-Esperon C, Garcia-Bermejo P, Ombelet F, McElduff P, Bivard A, Parsons M, Levi C. Evaluation of hyperacute infarct volume using ASPECTS and brain CT perfusion core volume. Neurology. 2017;88:2248–53.
Bivard A, Levi C, Krishnamurthy V, McElduff P, Miteff F, Spratt NJ, Bateman G, Donnan G, Davis S, Parsons M. Perfusion computed tomography to assist decision making for stroke thrombolysis. Brain. 2015;138(Pt 7):1919–31.
Souza LC, Payabvash S, Wang Y, Kamalian S, Schaefer P, Gonzalez RG, Furie KL, Lev MH. Admission CT perfusion is an independent predictor of hemorrhagic transformation in acute stroke with similar accuracy to DWI. Cerebrovasc Dis. 2012;33:8–15.
Campbell BC, Yassi N, Ma H, Sharma G, Salinas S, Churilov L, Meretoja A, Parsons MW, Desmond PM, Lansberg MG, Donnan GA, Davis SM. Imaging selection in ischemic stroke: feasibility of automated CT-perfusion analysis. Int J Stroke. 2015;10:51–4.
Bivard A, Kleinig T, Miteff F, Butcher K, Lin L, Levi C, Parsons M. Ischemic core thresholds change with time to reperfusion: a case control study. Ann Neurol. 2017;82:995–1003.
Lui YW, Tang ER, Allmendinger AM, Spektor V. Evaluation of CT perfusion in the setting of cerebral ischemia: patterns and pitfalls. AJNR Am J Neuroradiol. 2010;31:1552–63.
Lum C, Ahmed ME, Patro S, Thornhill R, Hogan M, Iancu D, Lesiuk H, Dos Santos M, Dowlatshahi D; Ottawa Stroke Research Group (OSRG). Computed tomographic angiography and cerebral blood volume can predict final infarct volume and outcome after recanalization. Stroke. 2014;45:2683–8.
Boned S, Padroni M, Rubiera M, Tomasello A, Coscojuela P, Romero N, Muchada M, Rodríguez-Luna D, Flores A, Rodríguez N, Juega J, Pagola J, Alvarez-Sabin J, Molina CA, Ribó M. Admission CT perfusion may overestimate initial infarct core: the ghost infarct core concept. J Neurointerv Surg. 2017;9:66–9.
Austein F, Riedel C, Kerby T, Meyne J, Binder A, Lindner T, Huhndorf M, Wodarg F, Jansen O. Comparison of perfusion CT software to predict the final infarct volume after thrombectomy. Stroke. 2016;47:2311–7.
Mokin M, Levy EI, Saver JL, Siddiqui AH, Goyal M, Bonafé A, Cognard C, Jahan R, Albers GW; SWIFT PRIME Investigators. Predictive value of RAPID assessed perfusion thresholds on final infarct volume in SWIFT PRIME (solitaire with the intention for thrombectomy as primary endovascular treatment). Stroke. 2017;48:932–8.
Haussen DC, Dehkharghani S, Rangaraju S, Rebello LC, Bouslama M, Grossberg JA, Anderson A, Belagaje S, Frankel M, Nogueira RG. Automated CT perfusion ischemic core volume and noncontrast CT ASPECTS (Alberta Stroke Program Early CT Score): correlation and clinical outcome prediction in large vessel stroke. Stroke. 2016;47:2318–22.
Padroni M, Boned S, Ribó M, Muchada M, Rodriguez-Luna D, Coscojuela P, Tomasello A, Cabero J, Pagola J, Rodriguez-Villatoro N, Juega JM, Sanjuan E, Molina CA, Rubiera M. CBV_ASPECTS improvement over CT_ASPECTS on determining irreversible ischemic lesion decreases over time. Interv Neurol. 2016;5:140–7.
Funding
This work was supported by the Health and Medical Research Fund research fellowship scheme of Hong Kong, grant number 01150027.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A.C.O. Tsang, S. Lenck, C. Hilditch, P. Nicholson, W. Brinjikji, T. Krings, V.M. Pereira, F.L. Silver and J.D. Schaafsma declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Tsang, A.C.O., Lenck, S., Hilditch, C. et al. Automated CT Perfusion Imaging Versus Non-contrast CT for Ischemic Core Assessment in Large Vessel Occlusion. Clin Neuroradiol 30, 109–114 (2020). https://doi.org/10.1007/s00062-018-0745-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-018-0745-6